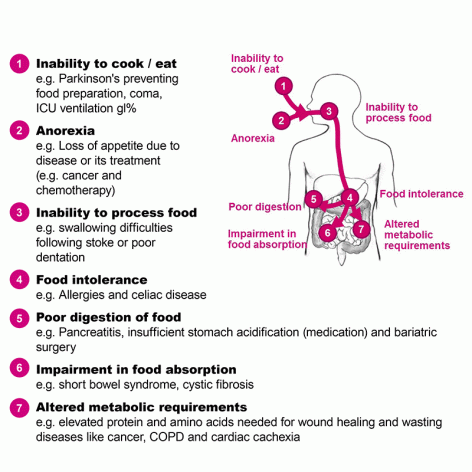
Malnutrition versus disease related malnutrition
Malnutrition (under nutrition) is a significant but often hidden problem. In the European community, it is estimated that 33 million people are at risk of becoming malnourished.2MNI MNI – Medical Nutrition Industry – www.Medicalnutritionindustry.com
It is well documented that these patients have poorer outcomes, e.g. they are3Stratton R, et al. Wallingford: CABI Publishing. Published on 2003 three times more likely to get an infection and 35% less likely to survive the full month after hospital admission.4Cereda, E, et al. Nutritional status in older persons according to healthcare setting: A systematic review and meta-analysis of prevalence data using MNA((R)). Clin Nutr. Published on 2016. 35(6): p. … Continue reading Furthermore, disease-related malnutrition negatively affects a patient’s quality of life. Patients can suffer from fatigue, loss of appetite, emotional and social functioning among other symptoms.
All of these affects can result in higher healthcare costs. The management of a malnourished patient is twice as expensive as a non-malnourished patient with 61% of patients who are malnourished increasing their hospital stay.5Khalatbari-Soltani, S. and P. Marques-Vidal, The economic cost of hospital malnutrition in Europe; a narrative review. Clin Nutr ESPEN, Published on 2015. 10(3): p. e89-e94

Undernutrition is often linked to an underlying condition or disease. Disease-related malnutrition is a condition characterized by inadequate intake of energy, protein, and/or micronutrients as a result of a diverse number of diseases or their treatment.7MNI MNI – Medical Nutrition Industry – www.Medicalnutritionindustry.com
Disease related malnutrition occurs when patients do not consume adequate quantities or quality of food from their diet or do not reach the right levels of nutrients to compensate for the specific nutritional needs created by the disease. Disease-related malnutrition can affect individuals at any life stage including infants and children, however the prevalence of malnutrition is significantly higher in the elderly and particularly common in healthcare settings.9Russell C and Elia M. Redditch, BAPEN. Published on 2008 ,10Russell C and Elia M. Redditch, BAPEN. Published on 2011 ,11Russell C and Elia M. Redditch, BAPEN. Published on 2012 One third of older people in hospital12Russell C and Elia M. Redditch, BAPEN. Published on 2008 ,13Russell C and Elia M. Redditch, BAPEN. Published on 2011 ,14Russell C and Elia M. Redditch, BAPEN. Published on 2012 ,15Imoberdorf, R, et al. Prevalence of undernutrition on admission to Swiss hospitals. Clin Nutr. Published on 2010. 29(1): p. 38-41 ,16Kaiser, M.J, et al. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc, Published on 2010. 58(9): p. 1734-8 ,17Vanderwee, K, et al. Malnutrition and nutritional care practices in hospital wards for older people. J Adv Nurs. Published on 2011. 67(4): p. 736-46 and more than one third of people living in care homes18Russell C and Elia M. Redditch, BAPEN. Published on 2008 ,19Kaiser, M.J, et al. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc, Published on 2010. 58(9): p. 1734-8 ,20Suominen, M.H, et al. How well do nurses recognize malnutrition in elderly patients? Eur J Clin Nutr. Published on 2009. 63(2): p. 292-6 ,21Lelovics, Z, et al. Results of nutritional screening in institutionalized elderly in Hungary. Arch Gerontol Geriatr . Published on 2009. 49(1): p. 190-6 ,22Parsons, E, R, Stratton, and M. Elia, An audit of the use of oral nutritional supplements in care homes in Hampshire. Proceedings of the Nutrition Society, Published on 2010. 69(OCE2) are considered to be at risk.
If patients are unable to meet their nutritional needs through their regular diet, they may benefit from taking medical nutrition products to either supplement their diet or as a sole source of nutrition if necessary. Dietary management with medical nutrition has been shown to be a safe and effective way to help patients to reach their nutritional target and improve patient outcomes including alleviating disease symptoms, aiding recovery from illness, regaining strength and improving quality of life. Dietary management of patients with medical nutrition also lowers patient care costs due to reduced complications, fewer hospitalisations and a reduced length of hospital stay.
View References
| 1 | Harris, D. and N. Haboubi, Malnutrition screening in the elderly population. J R Soc Med, Published on 2005. 98(9): p. 411-4 |
|---|---|
| 2, 7 | MNI MNI – Medical Nutrition Industry – www.Medicalnutritionindustry.com |
| 3, 6 | Stratton R, et al. Wallingford: CABI Publishing. Published on 2003 |
| 4 | Cereda, E, et al. Nutritional status in older persons according to healthcare setting: A systematic review and meta-analysis of prevalence data using MNA((R)). Clin Nutr. Published on 2016. 35(6): p. 1282-1290 |
| 5 | Khalatbari-Soltani, S. and P. Marques-Vidal, The economic cost of hospital malnutrition in Europe; a narrative review. Clin Nutr ESPEN, Published on 2015. 10(3): p. e89-e94 |
| 8 | Ljungqvist, O. and F. Man, Under nutrition: a major health problem in Europe. Nutr Hosp, Published on 2009. 24(3): p. 369-70 |
| 9, 12, 18 | Russell C and Elia M. Redditch, BAPEN. Published on 2008 |
| 10, 13 | Russell C and Elia M. Redditch, BAPEN. Published on 2011 |
| 11, 14 | Russell C and Elia M. Redditch, BAPEN. Published on 2012 |
| 15 | Imoberdorf, R, et al. Prevalence of undernutrition on admission to Swiss hospitals. Clin Nutr. Published on 2010. 29(1): p. 38-41 |
| 16, 19 | Kaiser, M.J, et al. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc, Published on 2010. 58(9): p. 1734-8 |
| 17 | Vanderwee, K, et al. Malnutrition and nutritional care practices in hospital wards for older people. J Adv Nurs. Published on 2011. 67(4): p. 736-46 |
| 20 | Suominen, M.H, et al. How well do nurses recognize malnutrition in elderly patients? Eur J Clin Nutr. Published on 2009. 63(2): p. 292-6 |
| 21 | Lelovics, Z, et al. Results of nutritional screening in institutionalized elderly in Hungary. Arch Gerontol Geriatr . Published on 2009. 49(1): p. 190-6 |
| 22 | Parsons, E, R, Stratton, and M. Elia, An audit of the use of oral nutritional supplements in care homes in Hampshire. Proceedings of the Nutrition Society, Published on 2010. 69(OCE2) |